One of the advantages of a career in roofing is that you work outside. This can be a pleasant experience in good weather, but can be dangerous under extreme conditions unless proper precautions are taken. The hazards of exposure to the elements fall under two broad categories: Cold Stress and Heat Stress.
1.1.5.1 Cold Stress
 Our bodies need to keep a core temperature of about 37°C (98.6°F). To prevent hypothermia and other consequences of a chilled core, your brain monitors temperature very closely. If the surface of your skin gets too cold, skin receptors send signals to the brain that your body needs to get warmer. Shivering is one way to warm up by making your muscles contract and expand in speedy bursts. This twitching motion produces heat, which helps to raise body temperature. It’s also how your brain tells you to get out of the cold and find warm shelter.
Our bodies need to keep a core temperature of about 37°C (98.6°F). To prevent hypothermia and other consequences of a chilled core, your brain monitors temperature very closely. If the surface of your skin gets too cold, skin receptors send signals to the brain that your body needs to get warmer. Shivering is one way to warm up by making your muscles contract and expand in speedy bursts. This twitching motion produces heat, which helps to raise body temperature. It’s also how your brain tells you to get out of the cold and find warm shelter.
Frostbite
If temperatures drop to freezing and below, the blood vessels close to exposed skin start to constrict in an attempt to keep the core of the body warm. When it is very cold, or exposure to cold is prolonged, blood flow to some parts of the body, for example the fingers and hands, can drop to dangerously low levels. Frostbite occurs when skin and underlying tissues freeze due to the lack of oxygen-rich blood to the affected area(s).
Any part of the body can be affected by frostbite, but most frequently, it affects the outer appendages—hands, ears, feet, nose and lips. Individuals who stay outdoors in the cold for prolonged periods are at risk of developing frostbite. The most common causes of frostbite are prolonged exposure to cold-weather conditions and from not wearing clothing suitable for the conditions. It can also be caused by direct contact with ice, freezing metals or very cold liquids or vapors. Exposed skin in cold, windy weather is most vulnerable to frostbite, but it can occur on skin covered by gloves or other clothing.
Frostnip is the first stage of frostbite. It doesn’t cause permanent skin damage and, if caught early enough, can be treated by warming your skin. Frostbite requires immediate medical attention. It can permanently damage skin, tissues, muscle and bones. Severe frostbite can lead to infection and nerve damage.
Wind Chill
In winter, one has to consider not only the air temperature, but also the wind chill. Wind chill involves the combined effect of air temperature and air movement. The wind-chill cooling rate is defined as heat loss (expressed in watts per meter squared) resulting from the effects of air temperature and wind velocity upon exposed skin.
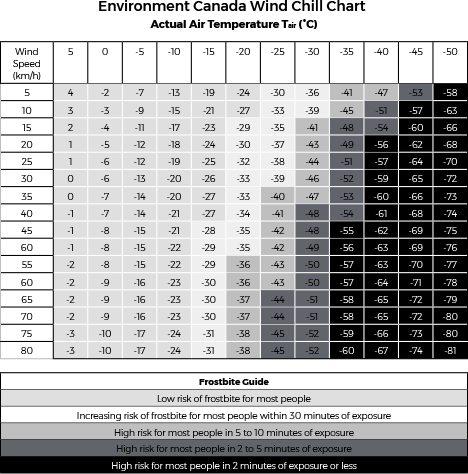
The higher the wind speed and the lower the temperature, the more rapidly the body will cool. The chart on the next page shows the effect of wind speed on temperature, commonly called the wind chill temperature. For any given combination of temperature and wind speed, the wind chill index corresponds roughly to the temperature that one would feel in a very light wind. For example, a temperature of -25°C (-13°F) and a wind speed of 20 km/h (12.4 mph) give a wind chill index of -37. This means that, with a wind of 20 km/h (12.4 mph) and a temperature of -25°C (-13°F), one would feel as if it were -37°C (-34.6°F) in a very light wind. Wind chill does not affect objects and does not lower the actual temperature. It only describes how a human being would feel in the wind at the ambient temperature. The wind chill index does not take into account the effect of sunshine. Bright sunshine may significantly reduce the effect of wind chill (make it feel warmer).
The box below the chart shows the risk of frostbite for given wind chill temperatures. As you can see at an air temperature of -20°C (-4°F) and a wind at 20 km/h (12.4 mph), frostbite to exposed skin will occur in approximately 30 min. If the temperature falls to -30°C (-22°F) and the wind increases to 40 km/h (25 mph), flesh will freeze in 2 to 5 minutes of exposure.
What to Do for Frostbite
- Move the person to a warm place.
- Handle the area gently; never rub the affected area.
- Warm gently by soaking the affected area in tepid water (38 to 41°C) (100.4 to 105.8°F) until it appears red and feels warm.
- Loosely bandage the area with dry, sterile dressings.
- If the person’s fingers or toes are frostbitten, place dry, sterile gauze between them to keep them separated.
- Avoid breaking any blisters.
- Do not allow the affected area to refreeze.
- Seek professional medical care as soon as possible.
Hypothermia
Hypothermia is the dangerous drop in body temperature, usually caused by prolonged exposure to cold temperatures. The risk of hypothermia is greatest in cold weather, but if you’re exposed to cold temperatures on a cool spring day, or get soaked from cold spring or fall rains, you can also be at risk of hypothermia.
Normal body temperature averages 37°C (98.6°F). With hypothermia, core temperature drops below 35°C (95°F). In severe hypothermia, core body temperature can drop to 28°C (82.4°F) even lower. As discussed previously, under cold conditions when the body can no longer maintain core temperature by constricting blood vessels, it shivers to increase heat production. However, this is limited to a few hours because of the depletion of muscle glucose (fuel) and the onset of fatigue.
Signs and Symptoms of Hypothermia
Mild hypothermia
- Core temperature of 37 to 35°C (98.6 to 95°F).
- Persistent shivering—usually starts when core temperature reaches 35°C (95°F).
- Blue lips and fingers.
- “Umbles” – stumbles, mumbles, fumbles, and grumbles which show changes in motor coordination and levels of Confusion and poor coordination have obvious effects on safety.
Moderate hypothermia
- Core temperature of 35 to 34°C (95 to 93.2°F).
- Loss of fine motor coordination, particularly in hands (e.g. cannot zip up coat, due to restricted peripheral blood flow).
- Violent shivering.
- Mental impairment and confusion.
- Slurred speech.
- Irrational behavior such as paradoxical undressing (e.g. person starts to take off clothing, and is unaware that they are cold).
- Demonstrates an “I don’t care” attitude.
- Heart slowdown.
- Slow breathing.
Severe Hypothermia
- Core temperature 33 to 30°C (91.4 to 86°F) degrees and below (immediately life threatening).
- Shivering occurs in waves; violent then pauses. Pauses get longer until shivering finally ceases as the heat output from burning glycogen in the muscles is not sufficient to counteract the continually dropping core temperature. The body shuts down on shivering to conserve glucose.
- Person falls to the ground, unable to walk, curls up into a fetal position to conserve heat.
- Muscle rigidity develops because peripheral blood flow is reduced and due to lactic acid and CO2 buildup in the muscles.
- Skin is pale.
- Pupils dilate.
- Pulse rate decreases.
At 32°C (89.6°F) the body tries to move into hibernation, shutting down all peripheral blood flow and reducing breathing rate and heart rate. At 30°C (86°F) the body is in a state of metabolic stasis. The person looks dead but is still alive.
What to Do for Hypothermia
- Call 911 or local emergency While waiting for help to arrive, monitor the person’s breathing. If breathing stops or seems dangerously slow or shallow, begin cardiopulmonary resuscitation (CPR) immediately.
- Move the person out of the If going indoors isn’t possible, protect the person from the wind, cover the head, and insulate the individual from the cold ground.
- Remove wet clothing. Replace wet things with a warm, dry covering.
- Keep the person awake.
- Do not apply direct Do not use hot water, a heating pad or a heating lamp to warm the person. Instead, apply warm compresses to the center of the body — head, neck, chest and groin. Do not attempt to warm the arms and legs. Heat applied to the arms and legs forces cold blood back toward the heart, lungs and brain, causing the core body temperature to drop. This can be fatal.
- Do not give the person alcohol. If conscious and if the person is not nauseous or vomiting, offer warm non-alcoholic drinks.
- Do not massage or rub the person. Handle people with hypothermia gently because their skin may be frostbitten, and rubbing frostbitten tissue can cause severe damage. Call 911 or local emergency number for medical help or transport casualty carefully to nearest medical facility.
1.1.5.2 Heat Stress
The busiest construction season is summer and roofers will often work long hours during the hot days of May through August. Working temperatures are often heightened significantly depending on roofing operations such as the application of hot asphalt in built-up roofing and the torching of modified bitumen membranes. Even without these operations, the roof can be a hot working environment. Studies have shown that temperatures on dark coloured roofs, such as traditional tar and gravel, can reach over 60°C (140°F) on a bright, still, sunny day. Light coloured roofs may not reach those high temperatures, but they can reflect the sun’s rays resulting in severe sunburn.
Workers who are exposed to extreme heat or work in hot environments may suffer serious illness and injury. Heat stress can result in heat stroke, heat exhaustion, heat cramps, or heat rashes. Heat can also increase the risk of injuries from sweaty palms, fogged-up safety glasses, and dizziness.
Your body is always working to keep a balance between how much heat it makes and how much it loses. Too much heat causes sweating. When the sweat evaporates from your skin, the surface of your body cools, and your temperature goes down. However, under some conditions, being hot for too long can be a problem. Heat stress can cause several illnesses grouped under the name hyperthermia.
Hyperthermia is elevated body temperature due to the body’s failure to regulate its core temperature. This occurs when a body produces or absorbs more heat than it can dissipate. Heat stress symptoms are a set of natural signals telling you that your body is unable to cool itself. When body temperature gets above 38-39°C (100.4 – 102.2°F), your brain starts to overheat. The body’s cooling system begins to shut down and your core temperature continues to rise. This can lead to extreme temperature elevation that becomes a medical emergency requiring immediate treatment to prevent disability or death.
Factors Influencing Heat Stress
The heating and cooling balance of the body depends on the following factors:
- Air temperature
- Humidity (moisture in the air)
- Radiant heat (sunshine, heat from hot tar, pavement, )
- Physical activity (how hard you’re working)
- Cooling (by the evaporation of sweat)
- Body adjustments (acclimatization)
There are two sources of heat exposure, the outside environment and internal muscle activity (80% of muscle energy is turned into body heat). High temperatures and high levels of physical work create heat stress. The body cools itself by evaporating sweat. High humidity hinders sweat from evaporating.
The body will get used to working in a hot environment gradually over time. Known as acclimatization, this occurs as the body becomes more efficient at cooling itself down. During this process:
- The body redirects blood to the skin’s surface.
- The heart becomes more efficient.
- Sweating starts sooner, and there is more of it.
- Sweat is less salty.
Acclimatized workers will generally be able to work longer in a hot environment. During this adjustment period, it is common to experience symptoms of fatigue, dizziness, heat rash, and stomach cramps. Acclimatization takes time — a rule of thumb for assuming you have acclimatized is when the last five of seven days have workplace temperatures in the heat stress range. It is important to remember that dehydration can defeat the process and any benefits of acclimatization.
Types of Heat Stress
Heat stress symptoms are a set of natural signals telling you that your body is unable to cool itself and your body temperature will increase. When body temperature gets above 38-39°C (100.4 – 102.2°F), the brain starts to overheat, leading to a shutdown of your body’s cooling system (sweating stops). Your temperature now rises even faster, leading to heat stroke and possibly death. The causes, symptoms, and treatment of various heat-related illnesses are listed below.
Heat Rash
Heat rash is a skin irritation caused by excessive sweating during hot, humid weather. A red, bumpy rash with severe itching, it is more likely to occur on the neck and upper chest, in the groin, under the breasts, and in elbow creases.
Workers experiencing heat rash should try to work in a cooler, less humid environment when possible. The affected area should be kept dry.
Sunburn
Too much exposure to the sun can cause red, painful, or blistering and peeling skin. If the skin blisters medical attention is needed. Skin lotions can help ease the pain. Avoid topical anaesthetics. Get out of direct sunlight.
Heat Cramps
Heat cramps usually affect workers who sweat a lot during strenuous activity. This sweating depletes the body’s salt and moisture levels. Low salt levels in muscles causes painful cramps in arms, legs, or the stomach. The cramps can occur suddenly while working or later, after you have left work.
Heat cramps are serious because they can be a warning of other more dangerous heat- induced illness such as heat exhaustion or heat stroke.
Workers experiencing heat cramps should stop all activity, loosen clothing and sit in a cool place. Drinking water alone will not replenish the salt your body needs, instead drink liquids with high electrolyte content (sports drinks, clear juices).
Do not perform any strenuous activity for a few hours after the cramps subside. Further exertion may lead to heat exhaustion, or heat stroke. If the heat cramps persist after an hour you should seek medical attention. If you suffer from heart problems, or are on a low-sodium diet you may be at risk for heat stroke and should get medical attention right away.
Heat Exhaustion
Heat exhaustion is the body’s response to an excessive loss of the water and salt, usually through excessive sweating. Workers who are elderly and /or have high blood pressure are particularly vulnerable to eat exhaustion.
Symptoms of heat exhaustion include:
- Heavy sweating
- Extreme weakness or fatigue
- Dizziness, confusion
- Nausea
- Clammy, moist skin
- Pale or flushed complexion
- Muscle cramps
- Slightly elevated body temperature
- Fast and shallow breathing
A worker suffering from heat exhaustion should immediately:
- Seek rest in a cool, shaded place, preferably an air-conditioned area.
- Drink plenty of water or other cool, non-alcoholic beverages.
- If possible, take a cool shower, bath, or sponge bath. If this isn’t feasible have someone spray cool water on you, or use cold wet compresses to help yourself cool down.
Heat Syncope (fainting)
Heat syncope is a fainting (syncope) episode or dizziness that usually occurs with prolonged standing or sudden rising from a sitting or lying position. It is usually the result of fluid loss, inadequate water intake, and lack of acclimatization.
Symptoms of heat syncope include:
- Lightheadedness
- Dizziness
- Fainting
Workers with heat syncope should:
- Sit or lie down in a cool place when they begin to feel symptoms.
- Slowly drink water, clear juice, or a sports beverage.
If sudden fainting after at least two hours of work coupled with cool moist skin and a weak pulse GET MEDICAL ATTENTION immediately. Fainting may also be due to other serious illnesses.
Heat Stroke
Heat stroke is the most serious heat-related disorder. It occurs when the body becomes unable to control its temperature: the body’s temperature rises rapidly, the sweating mechanism fails, and the body is unable to cool down. When heat stroke occurs, the body temperature can rise to 41°C (105.8°F) or higher within 10 to 15 minutes. Heat stroke can cause death or permanent disability if emergency treatment is not provided. If a person’s body has used up all its water and salt reserves, it will stop sweating, which can cause body temperature to rise; heat stroke may develop suddenly or may follow from heat exhaustion.
Symptoms of heat stroke include:
- Hot, dry skin or profuse sweating
- Hallucinations
- Chills
- Throbbing headache
- High body temperature
- Confusion/dizziness
- Slurred speech
Take the following steps to treat a worker with heat stroke:
- Call 911 or local emergency number and notify their supervisor.
- Move the sick worker to a cool shaded area.
- Cool the worker using methods such as:
- Soaking their clothes with water.
- Spraying, sponging, or showering them with water.
- Fanning their body.
Call for medical help immediately when a worker experiences high body temperature (above 41°C [105.8°F]) and any of the following:
- The person is weak, confused, upset, or acting strangely.
- The person has hot, dry, red skin; a fast pulse; headache or dizziness.
- The person passes out.
- The person has convulsions.
This condition can kill a person quickly and prompt action may save the person’s life.
